Symptoms and diagnosis
Steve, 60 from Reading, was a very fit and healthy 49-year-old when his life started to change and little did he know he would be embarking on a decade-long bowel cancer journey. He describes his story, starting with the beginning of his symptoms.

Steve pre-diagnosis
“During my 40s, I worked in pharmaceuticals as a Senior Manager at a leading UK pharmaceutical company then set up my consultancy practice eight years before I was diagnosed with bowel cancer to get a better work-life balance and avoid the high-stress environment I was constantly working in.
“I was very physically fit, doing 40-minute 10k runs, I was a mixed martial artist, regularly did yoga, was in the gym most days and had a relatively good diet. I was very fit, healthy and well and hadn’t been to the Doctor for over seven years.
“However my bowel habits slowly changed and I found myself frequently needing to go to the toilet but I had no pain or blood in my stools. I assumed it was down to a food allergy so I eliminated foods from my diet and took a few food tests but nothing came back as abnormal.
“On the whole, I felt OK, but on a couple of occasions, I felt very rough and drained from it. I was planning on racing on Exmoor and as soon as my friends saw how drained I looked, they said there was no way I could take part and I booked a GP appointment as soon as I could.
“I went to the GP and told the Doctor that I thought I had a bowel infection. The GP agreed with me and I was told to give a stool sample. I remember clearly the GP said, “Just to reassure you, this is not cancer” so I didn’t feel too worried.
“The stool test came back normal so another GP took a blood test which also came back normal. I still had the symptoms but no answer as to why. I was asked if I wanted more investigations, and I said yes as I didn’t feel right. I then saw a female GP who suggested I have a colonoscopy and at that point, I was starting to experience blood in my poo. I had a sigmoidoscopy booked where the clinician found piles and suggested that was the reason for the blood in my poo.
“I was meant to be flying to Las Vegas the weekend after the sigmoidoscopy and I naturally really wanted to go on the trip so I needed to know whether to wait until after a colonoscopy had been carried out but I was told I could wait a week until after my planned trip.
“After my trip, I went to the colonoscopy but the bowel prep didn’t work properly for the colonoscopy which was the first red flag. This was because the bowel prep normally works well and it is needed for a clear view in the colonoscopy.
“I was mildly sedated during the procedure but I was conscious and felt there was a lot of moving around to get the camera through the bowel. I was told there was an area of ulceration which they couldn’t get past with the camera. I was told I needed a CT scan and a biopsy and I saw a gastroenterologist a few days later who told me the results. I remember attending the appointment on my own as I was expecting a diagnosis of colitis.
“I was on my own with the nurse right next to me when I had the biggest shock of my life. I was told I had cancer which had spread to my cancer and lungs and remember thinking “That’s it then”. The gastroenterologist was so supportive and positive, that I was told I was fit and healthy and could handle an aggressive treatment plan, to ensure the best results. On the same day, I had an ultrasound on my liver to see the extent of the spread and was told they were tiny tumours but the one in the bowel was very large and about to obstruct the bowel and I needed surgery quickly.
“I drove home on my own from Slough to Maidenhead and that is when the tears started as it was such a huge shock. I got home and broke down, making almost guttural howls. My mental health was sinking quickly but I told myself to pull myself together, but the other side of me told me to get it out and to let me process the news.
“I then had a phone call from the surgeon on his mobile asking if I could come to his Maidenhead clinic straight away. He talked me through what was going to happen and explained we needed to get it out before it was obstructed otherwise I would lose the bowel. He had the right communication style and took the time to reassure me I was very fit and could handle the operation and treatment. The surgeon then kindly shared his own cancer journey and said ‘If I can do it, you can do it.’ The kindness made me think ‘OK, I could do this.’
Treatment
“The urgent operation was booked in quickly after a Bank Holiday weekend and I wondered how I would get through the long weekend alone with my thoughts. So I decided I needed to speak to people and explain what was going on.
“The first person I called was a close friend. At first, I couldn’t say the word ‘cancer’ or ‘and it’s spread’. But as I spoke to more people about it I was able to say the words. A few friends asked to come round and spent the night with me to keep me company and I soon realised it wasn’t only about me, the people around me were going through it too and I had to let people be involved in it. Over the weekend I realised I was entering a period where I was no longer going to be in control of my life.
“I had a lower abdominal resection which was successful. I was in hospital for a week and I remember waking up from the surgery and the recovery nurse kept saying the operation was a success and I didn’t have a stoma. She kept repeating it until I was aware of what was going on and responded and it was a relief.
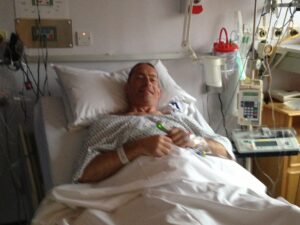
Steve post operation
“The next morning, the surgeon came into my room and said ‘Woah what a tumour, it was the biggest I have ever removed” which was quite an accolade. He told me I had a 20cm long, 6.5cm wide tumour which had grown along the bowel wall. He said it was the size of a large German sausage that they took out and it needed open surgery. Despite it not being laparoscopic surgery, he managed to connect the bowel back up without the need for a stoma. Within 3 days I was going to the toilet again and I had extra nights in the hospital as I live alone and needed a bit more care, but on the whole, it was a good experience.
“After the bowel resection, my mobility was restricted and then the intense chemo affected my day-to-day living. Friends came round to cook for me or take me out to places which worked well and was lovely. Going through stage 4 cancer brought me closer to my friends and family and really showed who my friends were.
“I learnt to ask for and accept help. I realised people wanted to help and our responsibility as the patient is to allow them to help. The patient needs to say, “This is what I need”.
Secondary tumours
“There were quite a few masses in my lungs which meant I was lucky I didn’t have more issues with my breathing. I remember looking at the scan and seeing the mushrooms appear over my lungs and I was told they couldn’t be operated on at that point. I needed 6 months of chemo and then a judgement on whether an operation would then be possible.
“I remember I didn’t want to be told the whole list of chemo side effects, then a couple of well-meaning friends told me their chemo horror stories which in hindsight was not helpful. I had a line put in which required tunnelling through the chest leaving a tube hanging from my chest (a Groshong Catheter) and I went in for chemo and was in the chair for about 8 hours.
“A friend of mine drove me to the hospital and I was scared, it looked like a room of old tatty chairs and very ill people. I felt rough and slept for some of it and my friend had to drive me home and cook for me as I had no energy and found it hard to eat that evening. The next morning I started to feel sick and remember thinking that this was what I’d been told about, and I was focussing on how bad this was going to be. Luckily I realised I was being so negative, and read some patient booklets which advised me to try to walk around and have toast and water to feel better. That made me think ‘Perhaps I can do this’. Since then I’ve become aware of something called the Nocebo Effect, where if you think something is going to do harm and not work then you are more likely to feel worse and chemo is the perfect example of this. I certainly experienced the nocebo effect.
“After three months of chemo, I found out that the lung secondaries were shrinking and after six months my liver was clear and my lungs were clear so I didn’t need more surgery. I felt very lucky despite having stage 4 cancer as I was diagnosed just before it spread. My bowel surgery was a great success as was the chemo and I hope this gives people hope.
“At that point I was told it was too early to know my prognosis and I needed to see how the chemo was going. I then asked what the prognosis was after my chemo and the oncologist said he can’t see beyond 1-2 years but he wanted to put me on maintenance chemo to control it and give me the best outcome.
Life now
“In a few weeks I celebrate the eleventh anniversary of my stage 4 cancer diagnosis! I live a full and active life, I’ve travelled;led all over the world including walking in the rainforest and practicing yoga in Bali!
After five years post-diagnosis I celebrated with a mini festival with 250 friends and live bands to celebrate. I did similar with my 10-year anniversary but it was more intimate. Over ten years after diagnosis I am on maintenance chemo and that is the reason I am still alive. I now see chemo as my friend. I now see it like an army coming to help me, it is not the enemy and I welcome it. Cancer is quiet whereas chemo is metaphorically loud and invasive, so it is easy to focus on the chemo as negatively.
“I have been on maintenance chemo for 10 years now and I would say life is normal. I am now doing a lot of advocacy and charity work in the cancer field, I’ve set up a project, www.striveforfive.org which aims to help share hope about stage 4 cancer. My life now is about friends and family and I am involved in medical education projects to help improve patient care, this includes writing whitepapers on areas like cancer communication which has had an incredible response in the medical community and is far-reaching and hopefully is helping to make a huge difference.
“I hope my story shows the importance of taking symptoms seriously and pushing for answers from the start then the importance of a positive mental attitude when going through chemotherapy. It is very easy to slide into negativity, but I always remind myself that chemo is my friend keeping me alive and no one should be afraid of it.”

Steve travelling recently

