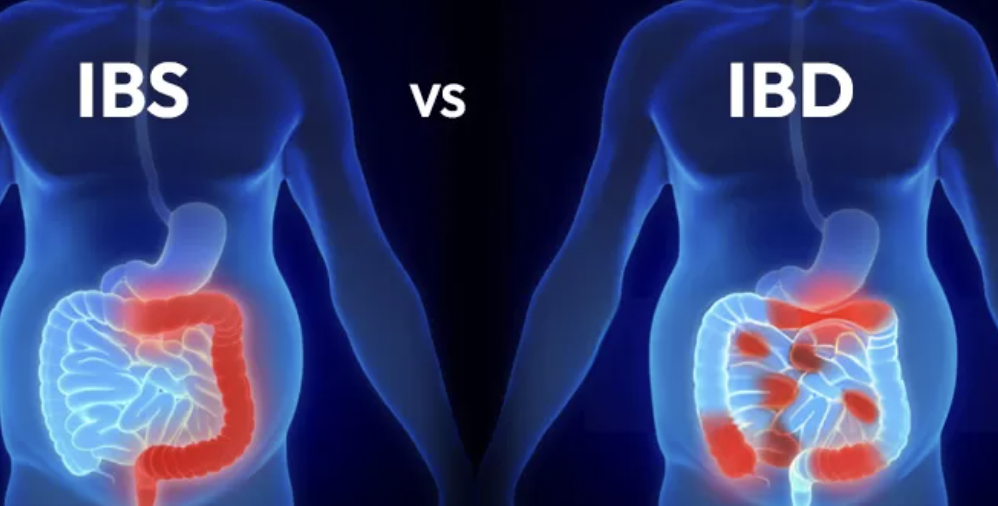
The terms Irritable Bowel Syndrome (IBS) and Inflammatory Bowel Disease (IBD) are often confused. Although they sound similar and can share similar symptoms, IBS and IBD are very different conditions with different causes, risks, and treatments. Understanding the distinction is
important for getting the right care and managing symptoms effectively.
What Is IBS?
Irritable Bowel Syndrome (IBS) is a functional gastrointestinal disorder. This means there is a
problem with how the gut works, not with its structure.
Common features of IBS:
● Abdominal pain or cramping
● Bloating and gas
● Dioarrhea, constipation, or alternating between both
● Symptoms that often improve after a bowel movement or a change in diet
IBS does not cause visible inflammation, ulcers, or damage to the intestines. Tests such as colonoscopies and blood samples usually appear normal.
What causes IBS?
The exact cause isn’t fully understood, but factors may include:
– Gut–brain communication issues
– Food sensitivities
– Stress and anxiety
– Changes in gut bacteria
IBS is chronic but not dangerous and does not permanently damage the intestines.
What Is IBD?
Inflammatory Bowel Disease (IBD) is a group of autoimmune conditions that cause chronic inflammation in the digestive tract. The two main types are:
- Crohn’s disease
- Ulcerative colitis
Common features of IBD:
– Persistent diarrhoea
– Abdominal pain
– Blood and/or mucus in stool
– Fatigue
– Weight loss
– Fever during flare-ups
– Bloating
– Extra-intestinal symptoms such as Arthritis, Osteoporosis, red and irritated eyes,
swellings of fat under the skin and mouth ulcers
Unlike IBS, IBD causes visible inflammation and tissue damage that can be seen on an endoscopy, and biopsies.
What causes IBD?
IBD is an autoimmune condition, meaning the immune system mistakenly attacks the digestive tract. Genetics, immune dysfunction, and environmental factors all play a role. IBD is a serious medical condition that can lead to complications such as intestinal strictures, fistulas, malnutrition, and an increased risk of colon cancer if not properly managed. There is no current cure for IBD, instead symptoms are managed to try and induce longer periods of remission, rather than periods of active symptom flare.
How Are They Treated?
IBS treatment focuses on managing symptoms and triggers:
– Dietary changes (such as a low FODMAP diet)
– Stress reduction
– Fibre, antispasmodics, or gut-targeted medications
IBD treatment focuses on reducing inflammation and preventing further damage:
– Anti-inflammatory medications
– Immunosuppressants
– Steroids during flare ups
Surgery in some cases
IBD treatments in Oxford
Oxford University Hospitals NHS Foundation Trust (OUH) is one the leading centres in Europe for the management of IBD; it has a dedicated IBD service with a multidisciplinary approach of specialist clinical and academic gastroenterology, specialist nursing, pharmacy, colorectal and paediatric departments working alongside ground breaking research teams at The Kennedy Institute of Rheumatology and NIHR Oxford Biomedical Research Centre.
Medical management treatment offered in Oxford include:
– Anti-inflammatory medication known as 5-ASA (aminosalicylates) compounds e.g.
Mesalazine
– Steroids such as Prednisolone
– “Biologics” medication: Anti-TNF (tumour necrosis factor) agents e.g Infliximab,
Adalimumab, Anti-integrin therapies e.g Vedolizumab, and IL-12/IL-23 (monoclonal
antibody) inhibitors e.g. Ustekinumab
Surgical intervention
– Colectomy: Surgery to remove part or all of the diseased area of colon with either a resection or stoma
– Stoma formation: creating an opening of the intestine on the outside of the body to bypass the inflamed area of colon either temporarily or permanently
– Ileo-Anal Pouch surgery: removing the inflamed part of the colon and forming an internal “pouch” using part of the small intestine
When to See a Doctor
If digestive symptoms are severe, persistent, or include blood in the stool, unexplained weight loss, severe abdominal pain, passing mucus, fever, or nighttime symptoms, it’s important to visit your GP. These are not typical of IBS and may indicate IBD or another serious condition.
Final Thoughts
While IBS and IBD can look similar on the surface, they are fundamentally different conditions. IBS affects quality of life but does not cause physical damage, whereas IBD is a chronic (life-long) inflammatory disease that requires ongoing medical treatment. Getting an accurate diagnosis is key to proper care and long-term health.
If you’re experiencing ongoing digestive symptoms, a healthcare professional can help determine the cause and guide you toward the right treatment plan.